Spinal Disorders: Fundamentals of Diagnosis and Treatment Part 111 potx
Bạn đang xem bản rút gọn của tài liệu. Xem và tải ngay bản đầy đủ của tài liệu tại đây (161.52 KB, 10 trang )
imaging is mandatory in order to determine salvage strategies in advance.
Hemostasis may be achieved by compression and packing.Ifthelesionoccurred
during drilling, a screw in the drill hole is a good option. The screw at the oppo-
site side, if not in place, should be skipped, and a salvage Gallie procedure can be
performed instead of using Magerl screws. Pseudoaneurysm and arteriovenous
fistulae are rare sequelae [61]. Stenting may be efficacious.
Posterior Approaches to the Thoracic and Lumbar Spine
Approach-related intraoperative complications are rare. Excessive bleeding can
occur. The risk is reduced by adequate patient positioning and change of platelet
inhibitors and anticoagulants to other drugs preoperatively. Very rarely, lesions
of anterior structures occur due to direct accidental stab trauma. Relatively rare
is an accidental lesion of the dural sac or of the spinal cord during preparation of
the approach. It is mandatory to use imaging to determine whether the posterior
vertebral elements are intact; otherwise, preparation has to be conducted with
more caution.
Procedure Related Complications
Decompressive Cervical and Lumbar Surgery
Check preoperative X-rays
for bony defects
Decompressive surgery in the cervical and lumbar spine is the most frequently
performed intervention but also prompts the need for revisions and surgery of
the adjacent segments. In some cases, complications can be avoided if the preop-
erative radiograph is checked for bony defects. In primary cases, this precaution
helps to avoid unintended dural lacerations (e.g., in spina bifida occulta).
Epidural Vein Bleeding
The blood loss may be considerable and can substantially reduce visualization,
compromising surgical success. Epidural bleeding usually stops after wound clo-
sure and turning the patient into the supine position. Reports on cauda equina
syndrome caused by postoperative continued epidural bleeding are rare [52].
Severe bleeding from epidural veins occurs in 3.5% in the hands of very experi-
enced surgeons, and in 7% in the hands of experienced surgeons [68].
Wash out Floseal after
epidural vein bleeding
has stopped
If severe bleeding occurs, it is sometimes better to continue removing the disc
herniation rather than attempting to coagulate the bleeding epidural vessels. Bleed-
ing often stops after removal of the disc herniation and facilitates exploration of the
bleeding vein. Compression of the vessel with a neurosponge allows the bleeding to
be controlled in the vast majority of cases. Generally, bipolar cauterization may be
necessary but should be limited because of postoperative scarring. Floseal is a very
efficient material to stop epidural bleeding. Usually, this agent increases its volume,
so that application in the vertebral canal requires caution. Removal of the agent by
irrigation is recommended when the bleeding has stopped.
Nerve Root Injuries
A nerve root may be damaged by:
malpositioning of a pedicle screw (
Fig. 4)
direct pressure or traction during decompression (e.g., PLIF procedures)
sharp instrumentation (high speed burrs)
cauterization (heat)
1104 Section Complications
ab
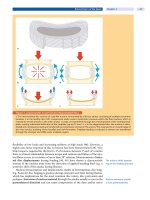
Figure 4. Malpositioning of a lumbar pedicle
a The axial CT scan shows that the pedicle screw has perforated the medial pedicle wall because of a far lateral recess.
b CT reformation of the images demonstrates that the screw has perforated the inferior medial aspect of the pedicle,
which hasled to a nerve root irritation. The pedicle was still intact after screw hole preparation with a blunt pedicle finder
(4 mm). However, the pedicle screw (7 mm) perforated the pedicle cortex, which was not noticed. In questionable cases,
it is recommended to again remove the screw after it has passed the pedicle and entered the vertebral body. However,
do not completely insert the screw if you want to remove it again to probe the pedicle because of the limited bony pur-
chase with screw reinsertion.
Poor visualization due to bleeding, perineural fibrosis, or congenital vertebral
(e.g., dysplastic pedicle) or neural abnormalities (conjoined nerve roots)
increases the risk of damage. The most vulnerable area for a lesion is the axilla of
the nerve root. Therefore, a good preventive principle is to stay lateral to the
nerve root when removing disc material [68]. Herniating root fibers have to be
reduced, and the defect has to be closed. However, a suture of the dura is very dif-
ficult and can cause stenosis. A fat or collagen pad or an artificial dura (e.g., Tis-
sueDura) with fibrin sealant is recommended to close the leak.
CaudaEquinaSyndrome
There are several reports on postoperative cauda equina syndrome after discec-
tomy for lumbar disc herniation [28, 52]. A frequent cause is extraction of a large
disc fragment through a small flavum window (microsurgical approach). The
syndrome is caused by direct pressure or by postoperative hematoma. A further
cause may be venous congestion in the presence of preexisting lumbar spinal ste-
nosis[52].Extendeddecompressionassoonaspossibleisrecommendedbut
recovery is often only partial.
Unintended Durotomy
The risk of unintended durotomy and cerebrospinal fluid (CSF) leaks can be
reduced with increasing surgical experience. However, sometimes minor tears
may become symptomatic only days or weeks after surgery (
Case Introduction).
Dural tears should be
repaired (if possible)
In severe spinal stenosis, which often presents with adhesions, dural tears occur
even in the hands of experienced surgeons. Closure of the defect is generally rec-
ommended. The following treatment options are available:
Treatment of Postoperative Complications Chapter 39 1105
Suture
Theleakshouldbecoveredwithaneurospongeuntiltherepairisperformed.The
leak can be sutured with non-resorbable 5-0 suture (interrupted or running) and
should be watertight. But care must be taken not to create a stenosis or suture in
a root fiber. It is debatable whether a small arachnoidal cyst should be opened
prior to the repair. In this setting, Gehri et al. [40] have reported a case in which
the suture of an arachnoidal cyst injured a small dural vessel and created a sub-
dural hematoma. It is advisable to control the tightness of the dural repair before
closing the wound. This is done either by tilting the table to increase the pressure
within the dura, or by high pressure respiration (increased PEEP). The muscle
fascia of the back muscles and the skin should be sutured so they are watertight.
Patch
If the dura is extremely thin or a large defect was created, the defect can be cov-
ered with fascia, muscle, fat, or synthetic material such as Tissue-Dura (Baxter),
Durepair (Medronic) or DuraGen (Integra). A fibrin sealant (e.g., Tissucol) can
be used to improve the closure. In complicated cases, however, a formal plastic
repair is necessary. In complicated cases, an external CSF drainage is necessary.
Leave It Open
Small CSF leaks often cause
more problems than large
defects
If there is no way to close the leak, it can be left open. In this case, it is absolutely
necessary to avoid formation of a CSF fistula, i.e., the wound closure must be
watertight. A pseudo-meningocele sometimes develops but usually does not
harm the patient. The CSF is very pervasive and will find its way out of the body.
A drainage (as overflow) is therefore recommended until the skin has healed.
Repair the dural defect
whenever possible
Antibiotic prophylaxis is recommended as long as there is drainage from the
wound or a drain is in-situ. In cases with adequate dural repair, bedrest is usually
not required. NSAIDs are administered for headache.
Lesions of Anterior Structures
Some case reports exist of intra-abdominal vascular or bowel injuries during
lumbar disc surgery [42, 44, 113]. Frequently, the stab wound is caused by a sharp
instrument or a rongeur (perforating the anterior anulus fibrosus). When using
a sharp instrument (e.g., chisel), the instrument has to be held tight to counteract
forces exerted by the hammer. The surgeon must always be aware that a structure
can suddenly break or is released jeopardizing underlying structures.
Anterior vessel injury by a
posterior approach is a life-
threatening complication
In the devastating situation of a major bleeding from an anterior vessel,the
patient has to be turned supine after compressing the wound with sponges as
effectively as possible. The posterior wound should be closed provisionally with
large stitches. The patient should immediately be positioned supine for an ante-
rior approach. Vessel repair must be done by the most experienced (vascular)
surgeon available.
Deformity Correction
Spinal Cord Injury
Spinal cord injury is the most serious complication and most frequently occurs in
deformity correction. There may be several reasons for spinal cord injury:
1106 Section Complications
Direct Spinal Cord Injury
Direct spinal cord injury
can occur by implants,
instruments or bony spurs
Direct injury may occur by improper placement of screws, hooks, sublaminar
wires, or may result from a fracture of the lamina, pedicle or posterior wall of the
vertebral body during correction maneuvers. Postoperative MRI may reveal
bleeding or ischemia in the spinal cord. Even delayed spinal cord injury can
occur due to compression by an implant in a narrow spinal canal [64]. For legal
reasons, the proportion of paraplegia caused by direct injury is not known. How-
ever, reports on neuromonitoring, where evoked potentials were restored after
implant removal, suggest that these cases exist.
Distraction
Distraction leading to spinal
cord injury is an avoidable
complication
Distraction may cause paraplegia especially in rigid angular curves, and in the
presence of malformations like diastematomyelia, where distraction of the spinal
cordcanmovethecordalongabonyorfibrousspurinthecord.Inmorethanhalf
of the cases of diastematomyelia combined with congenital scoliosis, a neurologi-
cal deficit can be found preoperatively [56].
Anterior Spinal Artery Syndrome
Anterior spinal artery syndrome is a devastating complication.Somatosensory
evoked potentials are likely to be false negative at the onset of the syndrome [7,
83], but motor evoked potentials will show the lesion immediately. It may be
caused by several mechanisms:
distraction
hypotensive anesthesia
vessel ligation
unknown causes
Avoid spinal deformity
correction in severe
hypotensive and
hypovolemic anesthesia
The blood flow in the anterior spinal artery can be decreased during distraction.
At least 65% of baseline blood flow is required to maintain spinal cord integrity
[83]. Hypotensive anesthesia or a sudden decrease of blood pressure may inter-
rupt sufficient oxygen supply of the motor fibers. In this condition, deformity
correction should be avoided until blood pressure and volume have been cor-
rected.
Vessel ligation cancauseanteriorspinalarterysyndromeinvascularsurgery
for aortic aneurysm. However, it is very unlikely to cause paraplegia in orthope-
dic cases, because in deformity surgery it is done unilaterally and on the convex-
ity of the curve. Nevertheless, it is recommended to provisionally clamp vessels
(control the effect with MEPs), ligate vessels only at the midvertebral level (collat-
eral supply), and to avoid hypotensive anesthesia.
Avoid low postoperative
hemoglobin and
hypotension after large
deformity correction
In a large study, not a single case of paraplegia was found in more than 1000
anterior operations [118]. In tumor resection, bilateral artery ligation may be
required,andtherearesomereportsofthesyndromeinthesecases[30].Para-
plegia especially due to anterior spinal artery syndrome can occur up to 3 days
after surgery [107]. In cases with large deformity corrections, low postoperative
hemoglobin and hypotension should be avoided to allow for an adequate vascu-
larization of the spinal cord, which may be compromised by the correction [51].
Treatment of Postoperative Complications Chapter 39 1107
Reduction of High-Grade Spondylolisthesis
Neural Injuries
In high-grade spondylolisthesis (see Chapter 27 ), particularly the L5 nerve root
is at risk. The incidence depends on the surgical technique and may be higher
than 50% if full reduction is attempted [14]. More than 50% of the lesions resolve
with time. The nerve root lesion can become clinically apparent even hours after
the completion of the operation. Neural compromise can occur by three mecha-
nisms:
cauda equina compression
foraminal impingement
nerve root stretching
Avoid complete correction
of high-grade spondylolis-
thesis
A cauda equina syndrome can occur as a result of a compression over the poste-
rior edge of the sacral dome after in situ arthrodesis with or without decompres-
sion [75]. Immediate decompression including resection of the dorsoapical rim
of the sacral dome is recommended [103]. Foraminal stenosis is a frequent find-
ing in high-grade spondylolisthesis [63]. Correction of the lumbosacral kyphosis
reduces the foramen even more. Sagittal translation of the slipped vertebra
causes a non-linear nerve root stretch (70%ofthestretchoccursafterareduc-
tion of more than 50%) [91]. It is therefore recommended to avoid a correction
of more than 50%.
Major Bleeding
Complete corpectomy
in high-grade spondylo-
listhesis may lead
to life-threatening
uncontrollable bleeding
In Gaines procedures (complete corpectomy of the slipped vertebra), life-threat-
ening bleeding can occur from the pre-sacral venous plexus.Spongesandhemo-
static agents (
Table 6) can be used to control bleeding.
Corpectomy/Osteotomy
Excessive Bleeding from Bone
Blood loss during corpectomy and osteotomy can be excessive and can rapidly
cause hemodynamic problems. Control of bleeding by compression with sponges
is the first method which creates time for further planning. If the bleeding is from
cancellous bone, bone wax and hemostatic agents are helpful (
Table 6). In cases
of arterial or venous injuries from major vessels, the outline recommendations
above apply.
Excessive Tumor Bleeding
Always prepare the
instrumentation prior
to tumor removal
The optimal way to prevent bleeding is by preoperative embolization [45, 82, 87].
However, this is not always possible. Resection should always start in areas not
affected by the tumor (e.g., the intervertebral disc), and instrumentation (e.g.,
screw placement and unilateral rod implantation) should be prepared to allow
for a rapid determination of the surgery in the case of hemodynamically relevant
bleeding. If bleeding occurs, a practical approach is to remove the tumor as
quickly as possible, and then to control the bleeding. However, this must be
planned and coordinated with the anesthetist. It is not wise to start tumor
removal when the patient is hemodynamically unstable.
1108 Section Complications
Postoperative Complications
Surgery does not end
with skin closure
Postoperative management is a decisive factor for the success of the surgery. It
must be structured and a close communication between the involved specialists
is mandatory.
P ost operative monit oring should follow a protocol with regard to:
blood loss
required laboratory analyses
neurological examinations
vascular examinations
Threshold values for action must be defined (blood loss per hour), as well as
pathways for examination in the case of bleeding or a neurological deficit.
Homeostasis Related Complications
Postoperative Bleeding
The amount of blood loss varies considerably with the surgical intervention. In
the case of significant or unexpected blood loss detected either by loss through a
drainage system or a decrease of hemoglobin concentration, a vital level of
hemoglobin has to be maintained, and the cause of bleeding must be assessed.
The minimal accepted hemoglobin concentration depends on age, comorbidity
andtypeofsurgery.Asarule,6–7g/dlcanbeacceptedinchildrenand8–10g/dl
in elderly people without comorbidity. However, it is important to individually
define the minimally accepted hemoglobin concentration based on the patient’s
general condition and type of procedure (e.g., deformity correction). In elderly
people, the individual risk of stroke, cardiac failure and renal failure must be con-
sidered.
A threshold amount (e.g., 600 ml/h) of blood loss from a chest tube or suction
drain is difficult to define and depends on:
The indications for when
to revise depend on the
patient and type of surgery
body weight
age
homeostasis
hemoglobin
confounding diseases
availability of blood
surgical situation
A coagulopathy or bleeding from a large, perhaps tumor infiltrated wound area
cannot be controlled by surgery alone. An unexpected major bleeding,not
caused by a coagulopathy, requires imaging, i.e.:
angiography
contrast CT
Angiog raphy is the best choice, because interventional closure of a vessel can be
performed. Segmental vessels of the spine and vessels supplying a tumor can be
occluded by subsequent coil embolization or stent implantation. Contrast CT
scan is less time consuming than angiography, and also provides information
about the bleeding site. This method is preferred if bleeding from a large vessel in
the pelvis is suspected, and if the cardiovascular status of the patient allows a
delay.
Treatment of Postoperative Complications Chapter 39 1109
Postoperative Hematoma
In posterior approaches, hematomas normally do not cause major problems. The
patient is usually lying supine in the early postoperative course, and the pressure
of body weight on the posterior wound does not allow large hematomas to
develop. The rate of infection in large hematomas is not established, so that clear
guidelines of when to evacuate a hematoma cannot be drawn up. Even evidence
to use or not to use a closed suction drain is lacking [89].
Retroperitoneal Hematoma
The retroperitoneal space can contain 3-4 L of blood, and can cause an ileus,
which can usually be treated conservatively. If bleeding has stopped, evacuation
will be necessary only in rare cases.
Epidural Hematoma with Neurological Deterioration
Epidural hematoma causing
cauda equina compression
requires urgent
decompression
Extradural hematomas can be seen relatively often in MRI scans after decom-
pressive surgery but seldom cause compression. Immediate decompression is
required in case of a cauda equina syndrome. In elderly patients with extensive
decompression, thromboembolic prophylaxis should be started postoperatively
instead of preoperatively as a preventive measure (although not evidence based).
Neurological Complications
A thorough postoperative
neurological examination
is a must
It is self-evident that a thorough neurological examination must be performed as
soon as the patient is fully awake. Neuromonitoring helps but cannot completely
avoid neurological complications.
Nerve Root Injury
If a nerve root injury is discovered postoperatively, analysis is preferably done by
MRI scan. A CT scan can show the position of pedicle screws more precisely than
MRI. Malpositioning of a pedicle screw must be corrected as soon as possible.
Spinal Cord Compromise
In the SRS Morbidity and Mortality Report 2003, the incidence of developing a
complete paraplegia was 0.1% related to all spinal operations, and 0.2% for incom-
plete paraplegia. Delayed paraplegia developing in the first three postoperative
days is rare but does occur [107]. Hypotension, hypovolemia and anemia should be
avoided in patients who have undergone major corrective surgery. In case of a spi-
nal cord syndrome, rapid assessment of potential causes is self-evident. Spinal
cord compression can occur due to an epidural hematoma, implants (hooks, mal-
positioning of pedicle screws), bone cement after vertebroplasty, and homeostatic
material (
Table 6
). In case of deformity correction, the correction must be released
butitremainsamatterofdebatewhetherallimplantsmustberemoved.
Postoperative Wound Problems
In case of postoperative
fever, rule out wound, lung,
urinary tract and catheter
infection
The prevailing symptom of a wound infection in the immediate postoperative
period is:
fever
1110 Section Complications
However, an elevated temperature (<39°C) up to the third postoperative day is
not worrisome and is most often related to a hematoma resorption or postopera-
tive aggression syndrome, although infection parameters should be determined
as a baseline and allow the further course to be judged.
According to the CDC (Center for Disease Control and Prevention) classifica-
The differentiation of
superficial and deep spinal
infections is arbitrary
tion, superficial and deep infections are differentiated. A superficial infection is
located in the skin and subcutis, and a deep infection below the muscle fascia.
Wound erysipelas is a special form of superficial cutaneous infection, e.g., strep-
tococci spread by the lymphatic system. Deep infections may be dependent on
the presence of an implant [57]. Ultrasonography with needle aspiration can be
helpful to distinguish between deep and superficial infection [67]. CT scans with
contrastmediaorMRIscansareoftenusedtodemonstrateinfections,butthere
is no evidence on the sensitivity or specificity available. There is also a lack of
published data on the ability of imaging methods to distinguish between hema-
toma and infected hematoma. There is a considerable variation in the number of
surgeons applying CDC categories [117]. It is also not possible to recommend
In equivocal cases always
explore and debride the
entire field of surgery
eitherexplorationoftheentirewoundineveryinfectionortotreataninfection
as a superficial infection until direct proof of a deep infection. The probatory
inspection may bring bacteria into contact with an implant if the infection was in
reality suprafacial, and in other cases proper treatment of a deep infection may
be postponed.
Superficial Infection
This may cause prolonged wound healing, and occurs in 2–3% of cases in lum-
bar discectomy [93], 0.9% in lumbar fusion [38] and in more than 5% in pediat-
ric patients with deformities due to cerebral palsy [109]. In the study by Szoke et
al. [109], all superficial infections were treated successfully by antibiotics and
local wound care. To prevent a superficial infection, pressure to the skin must be
avoided, and also the use of electrocoagulation for skin dissection may increase
the risk. Before systemic antibiotic administration, a culture shouldbetakenby
Deep biopsies provide
a more reliable result
than a swab
aswaborbetteradeep biopsy. Treatment depends on the cause. A widespread
infection, especially erysipelas, is treated by antibiotic administration. Fre-
quently, excision of the wound, mobilization of the skin and re-sutures are the
best way to achieve early healing.
Deep Infection
Deep infections occur in 2.4% of spinal fusions [38], and more than 4% in pedi-
atric patients with deformities due to cerebral palsy [109], and are treated by
debridement, irrigation or hardware removal. Early debridement is especially
recommended after instrumented fusion, when clear signs of deep infection are
found. Otherwise, biofilm-forming bacteria (staphylococci) can only be elimi-
nated by implant removal. Implant removal of long posterior instrumentations
and subsequent use of a brace causes loss of correction [92]. Reinstrumentation
Titanium implants are less
susceptible to infections
and can be left in situ after
debridement
in a single stage intervention reduces this risk [80]. Titanium implants appear to
be less susceptible to infection than stainless steel implants and can remain in
placeifaradicaldebridementofthewoundisperformed.
Spondylodiscitis
Spondylodiscitis may occur after discography and intradiscal procedures. A
dural abscess may develop. Fever and severe back pain or neck pain can arise in
the first postoperative days. Persistent or increasing back pain after intradiscal
Treatment of Postoperative Complications Chapter 39 1111
procedures with or without increased infectious parameters should prompt the
suspicion of a discitis. Incidence is less than 1% [46, 53, 96, 98]. MRI is the imag-
ing modality of choice. Subsequent to a biopsy to determine the germ, systemic
antibiotic treatment is usually sufficient. Even an epidural abscess without neu-
rological symptoms can be treated this way. A psoas abscess or a paraspinal
abscess can be drained after percutaneous puncture either under ultrasound or
CT guidance. Outcome is usually good but about 50% progress to spontaneous
interbody fusion [76]. Open surgical treatment follows the rules outlined in
Chapter
36 .
Persistent Wound Drainage
Rule out infection in case of
persistent wound drainage
The cause of this is either infection or a seroma. Ultrasound or other imaging
methods can be used for differentiation. Low serum albumin concentration can
contribute as well but it is debatable whether substitution of albumin is helpful.
Treatment options for postoperative seromas and persistent drainage include
observation for spontaneous resolution, external compression by bandages, and
wound revision with the aim of closing an empty space. Frequent wound disin-
fection and proper wound dressing diminish the risk of secondary infection.
Cerebrospinal Fluid Fistula
Small leaks often cause
more problems than large
defects
In the case of wound drainage, a CSF leak must be excluded. The diagnosis of a
CSF leakage does not cause diagnostic problems if a clear fluid drainage is seen.
In unclear cases, the glucose concentration can be determined (50–80 mg/
100 ml), which is much higher than in a seroma. The CSF production is about
500 ml/day and drainage can therefore be considerable. Intermittent CSF loss
causes neck stiffness (in 83%), headache (87%), nausea, and dizziness. Headache
will get worse in the upright position, and is ameliorated in the supine position.
This so-called hypoliquorrhea syndrome (
Case Introduction)ismostoften
observed in small lesions which form a valve mechanism and hardly ever occur
with large defects.
The principles of treatment have been outlined above. In uncomplicated cases,
asimplestitchoverthepartofthewoundwheretheCSFisleakingsuffices.Pro-
phylaxis with antibiotics which pass the blood-brain barrier are recommended
until wound secretion has stopped and all drains are removed.
Vascular Complications
Postoperatively or after angiographic interventions, the arteries have to be moni-
tored. In arteries supplying the legs, a pulse oximeter can be used for monitoring,
andthelegcompartmentshavetobecontrolledaswell.Arterial thrombosis
should be managed as an absolut e emergency case.
Postoperative Venous Thrombosis
In a recent review by Baron and Albert [5], the rate ranged between 0.3% and 1%
with the exception of a single study on a small sample size. In a Japanese study
containing 3499 patients, it was only 0.1% [85]. In neurosurgical procedures in
2643 patients and by use of duplex ultrasound scanning, the rate was 6%, 8% in
craniotomy and 1.5% in cervical and lumbar spine procedures. Of these, 90%
had malignant neoplasms, and 70% had lower-extremity neuromotor dysfunc-
tion [36]. Epstein [32] concluded that low molecular weight heparin should be
recommended for prevention, but its use must be weighed against the risk of
1112 Section Complications
hemorrhage. The duration of prophylaxis remains unclear. Our recommendation
is to administer a thromboembolic prophylaxis during the hospital stay and in
high risk patients (tumors, paralysis). If a venous thrombosis is suspected (swol-
len leg, pain), duplex ultrasound is recommended. Treatment is the administra-
tion of LMWH and compression stockings for at least 3 months.
Pulmonar y Problems
Pulmonary Embolism
Therateoffatallung
embolism after spinal
surgery is very low
Fatal long embolism is extremely rare. According to the Morbidity and Mortality
Report of the Scoliosis Research Society [21], the rate of fatal pulmonary embo-
lism (PE) is 0.02 %.Thetruerateofnon-fatalPEmaybeunderestimatedbecause
of a subclinical course. The rate may vary between 0.5% (posterior surgery) and
6% (combined anterior/posterior surgery) for adult spinal surgery [23]. Typical
signs of PE are:
chest pain
pulse acceleration
insufficient oxygenation
Diagnosis of central pulmonary embolism is made by multi-slice CT scan, and
treatment is usually by high dose low molecular weight heparin.
Pneumonia
The incidence of pneumonia after spinal interventions for adult spinal deformity
correction ranges between 1% and 3.6% [5]. Antibiotic treatment is usually suf-
ficient. Overdosage of opioids in elderly patients can result in aspiration pneu-
monia. A progression of pneumonia to an adult respiratory distress syndrome
(ARDS) is very rare but can be lethal.
Gastrointestinal Problems
Postoperative Bowel Atonia
A large retroperitoneal
hematoma increases the risk
of a paralytic ileus
Bowel atonia is a common problem after anterior lumbar approaches and usually
lasts for 3–5 days. A large retroperitoneal hematoma and a low serum potassium
level increase the risk of paralytic ileus. Symptoms are abdominal pain and vomi-
ting. Prevention includes minimal invasiveness of the intervention, early oral
feeding [95, 100], peroral fluids on the day of surgery, restriction of intravenous
fluid substitution to 2000 ml, and early mobilization of the patient. There is no
evidence that feeding has to be stopped until bowel movement has started. Treat-
ment is by replacing opioid treatment by NSAIDs. Colon stimulating laxatives
based on bisacodyl and magnesium are recommended, but there are no prospec-
tive trials to support this recommendation. The intravenous administration of
metoclopramide or cholinesterase inhibitors (distigmine bromide, pyridostig-
mine bromide) has shown no effect on reducing the duration of postoperative
ileus in any of the prospective studies [17].
Cast Syndrome/Superior Mesenteric Artery Syndrome
Cast syndrome may result
from kyphosis correction
and must not be missed
After correction of a deformity, especially after correction of kyphosis, the
ascending duodenum may be compressed between the stretched aorta and the
superior mesenteric artery. The patient vomits after swallowing food. Under-
Treatment of Postoperative Complications Chapter 39 1113